Advanced Diagnosis and Treatment for Melanoma in New Jersey
Melanoma is one of the most serious and potentially life-threatening forms of skin cancer, though it accounts for only about 1% of all skin cancer cases in the United States. Unlike basal cell carcinoma and squamous cell carcinoma, melanoma has a higher likelihood of spreading (metastasizing) to other organs if left untreated. The good news is that melanoma is highly treatable when detected early. At Skin & Laser Center of NJ, our board-certified dermatologists provide expert diagnosis, advanced treatment options, and ongoing support to help patients protect their health and maintain peace of mind.
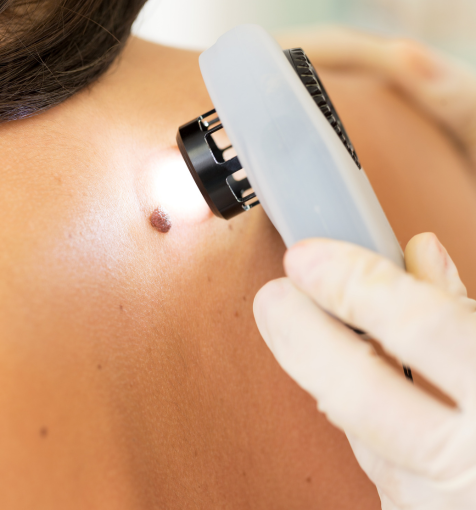

Melanoma begins in the pigment-producing cells of the skin called melanocytes. While it may arise from a previously existing mole, it can also develop as a new spot on otherwise normal-looking skin. Risk factors for melanoma include:
Excessive UV exposure: From sunlight or tanning beds
Family history: Having close relatives with melanoma increases risk
Fair skin: Especially with light hair or eye color and a tendency to burn easily
Multiple moles: Particularly atypical or irregular ones
Weakened immune system: Making it harder to fight abnormal cell growth
Because melanoma can progress quickly, patients are encouraged to schedule routine skin checks and promptly report any suspicious changes. Early detection dramatically improves treatment outcomes.
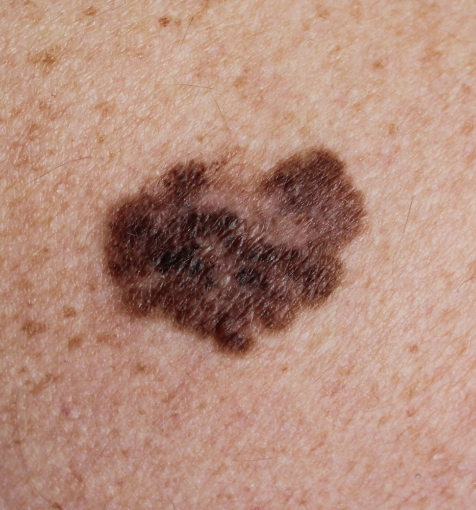
Patients can play an active role in spotting melanoma early by using the “ABCDE” guidelines when checking their skin:
A – Asymmetry: One half of the mole does not match the other
B – Border: Irregular, blurred, or jagged edges
C – Color: Uneven shades of brown, black, red, white, or blue
D – Diameter: Larger than 6 millimeters (about the size of a pencil eraser)
E – Evolving: Any change in size, shape, color, or sensation
If you notice any mole or blemish that fits these criteria, or if a lesion begins to itch, bleed, or look different from others, it’s important to seek professional evaluation right away. Our dermatology team uses advanced diagnostic tools, including dermoscopy and biopsy, to confirm or rule out melanoma.
Treatment for melanoma depends on the stage and severity of the cancer, as well as its location and size. Options at Skin & Laser Center of NJ may include:
Surgical excision: Removal of the melanoma and a margin of surrounding skin to ensure complete clearance
Mohs surgery: In certain cases, especially for melanoma in situ (early-stage), this technique allows for precise removal while sparing healthy tissue
Lymph node evaluation: If melanoma is advanced, nearby lymph nodes may be examined to determine if cancer has spread
Collaboration with oncology: For advanced cases requiring immunotherapy, targeted therapy, or chemotherapy, we coordinate closely with cancer specialists to provide comprehensive care
Our approach prioritizes early intervention, patient safety, and cosmetic outcomes, ensuring the best possible results for both health and quality of life.
Learn More About Melanoma
Melanoma treatment at Skin & Laser Center of NJ begins with a diagnosis. Your provider will first carefully examine moles and other suspicious spots. To get a better look, they may use a device called a dermatoscope, which shines light into the skin and allows them to see into the lesion so that they can evaluate the pigment pattern and other structures in the skin.
If a mole or other spot that looks suspicious is identified, they will remove tissue via biopsy and send it to a lab for microscopic evaluation. Melanoma can’t be diagnosed without a biopsy. Biopsies are quick, safe, and easy for a dermatologic specialist to perform.
After a diagnosis is confirmed, there are several treatment options. We will work with you to choose the best treatment plan based on the stage, location, and size of the melanoma, as well as your overall health.
Treatment options at Skin & Laser Center of NJ typically include surgery, though several methods exist.
When treating melanoma, we want to remove all of the cancer. If the cancerous cells have not spread, it is often possible to remove the melanoma during an office visit. If caught early, this may be the only treatment needed. The patient typically remains awake during the surgical procedure. There are multiple types of surgery:
The provider numbs the skin with a local anesthetic, then surgically removes the melanoma along with a rim of normal-looking skin. This normal-looking skin is called a margin. Most of the time, this procedure can be performed in the office.
This procedure is only applicable for early melanoma of the head and neck. The specially trained Mohs surgeon first numbs the skin with a local anesthetic, then removes the visible part of the lesion, which is processed for examination under a microscope to look for cancer cells. This layer-by-layer approach continues until the surgeon no longer finds cancer cells. In most cases, Mohs surgery can be completed within a day or less.
Other treatments for more advanced melanoma may also include:
Patients who have a different type of skin cancer, such as basal cell carcinoma or squamous cell carcinoma, may benefit from another approach. The key is to start with a diagnosis to determine the type of cancer, its stage, and other details that will help to determine which treatment would be best.
Convenient walk in hours available below. No appointment needed! Accepting private insurance and medicare. No medicaid plans.
Learn more about medical treatments at New Jersey’s Skin & Laser Center of NJ. Call 201-500-7525 or contact us online to schedule a consultation.